NEET MDS Lessons
Orthodontics
Growth is the increase in size It may also be defined as the normal� change in the amount of living substance. eg. Growth is the quantitative aspect and measures in units of increase per unit of time.
Development
It is the progress towards maturity (Todd). Development may be defined as natural sequential series of events between fertilization of ovum and adult stage.
Maturation
It is a period of stabilization brought by growth and development.
CEPHALOCAUDAL GRADIENT OF GROWTH
This simply means that there is an axis of increased growth extending from the head towards feet. At about 3rd month of intrauterine life the head takes up about 50% of total body length. At this stage cranium is larger relative to face. In contrast the limbs are underdeveloped.�
By the time of birth limbs and trunk have grown faster than head and the entire proportion of the body to the head has increased. These processes of growth continue till adult.��
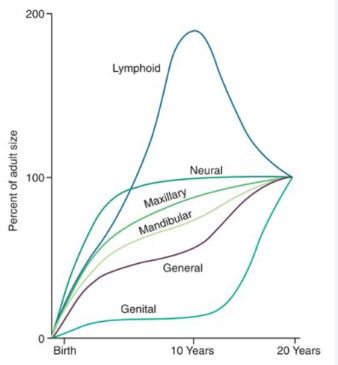
SCAMMON�S CURVE
In normal growth pattern all the tissue system of the body do not growth at the same rate. Scammon�s curve for growth shows 4 major tissue system of the body;
� Neural
� Lymphoid�
� General: Bone, viscera, muscle.
� Genital
The graph indicates the growth of the neural tissue is complete by 6-7 year of age. General body tissue show an �S� shaped curve with showing of rate during childhood and acceleration at puberty. Lymphoid tissues proliferate to its maximum in late childhood and undergo involution. At the same time growth of the genital tissue accelerate rapidly.�
�
Biology of tooth movement
1. Periodontal Ligament (PDL)
- Structure: The PDL is a fibrous connective tissue that surrounds the roots of teeth and connects them to the alveolar bone. It contains various cells, including fibroblasts, osteoblasts, osteoclasts, and immune cells.
- Function: The PDL plays a crucial role in transmitting forces applied to the teeth and facilitating tooth movement. It also provides sensory feedback and helps maintain the health of the surrounding tissues.
2. Mechanotransduction
- Mechanotransduction is the process by which cells convert mechanical stimuli into biochemical signals. When a force is applied to a tooth, the PDL experiences compression and tension, leading to changes in cellular activity.
- Cellular Response: The application of force causes deformation of the PDL, which activates mechanoreceptors on the surface of PDL cells. This activation triggers a cascade of biochemical events, including the release of signaling molecules such as cytokines and growth factors.
3. Bone Remodeling
- Osteoclasts and Osteoblasts: The biological response to
mechanical forces involves the coordinated activity of osteoclasts (cells
that resorb bone) and osteoblasts (cells that form new bone).
- Compression Side: On the side of the tooth where pressure is applied, osteoclasts are activated, leading to bone resorption. This allows the tooth to move in the direction of the applied force.
- Tension Side: On the opposite side, where tension is created, osteoblasts are stimulated to deposit new bone, anchoring the tooth in its new position.
- Bone Remodeling Cycle: The process of bone remodeling is dynamic and involves the continuous resorption and formation of bone. This cycle is influenced by the magnitude, duration, and direction of the applied forces.
4. Inflammatory Response
- Role of Cytokines: The application of orthodontic forces induces a localized inflammatory response in the PDL. This response is characterized by the release of pro-inflammatory cytokines (e.g., interleukins, tumor necrosis factor-alpha) that promote the activity of osteoclasts and osteoblasts.
- Healing Process: The inflammatory response is essential for initiating the remodeling process, but excessive inflammation can lead to complications such as root resorption or delayed tooth movement.
5. Vascular and Neural Changes
- Blood Supply: The PDL has a rich blood supply that is crucial for delivering nutrients and oxygen to the cells involved in tooth movement. The application of forces can alter blood flow, affecting the metabolic activity of PDL cells.
- Nerve Endings: The PDL contains sensory nerve endings that provide feedback about the position and movement of teeth. This sensory input is important for the regulation of forces applied during orthodontic treatment.
6. Factors Influencing Tooth Movement
- Magnitude and Duration of Forces: The amount and duration of force applied to a tooth significantly influence the biological response and the rate of tooth movement. Light, continuous forces are generally more effective and less damaging than heavy, intermittent forces.
- Age and Biological Variability: The biological response to orthodontic forces can vary with age, as younger individuals tend to have more active remodeling processes. Other factors, such as genetics, hormonal status, and overall health, can also affect tooth movement.
Functional Matrix Hypothesis is a concept in orthodontics and craniofacial biology that explains how the growth and development of the craniofacial complex (including the skull, face, and dental structures) are influenced by functional demands and environmental factors rather than solely by genetic factors. This hypothesis was proposed by Dr. Robert A. K. McNamara and is based on the idea that the functional matrices�such as muscles, soft tissues, and functional activities (like chewing and speaking)�play a crucial role in shaping the skeletal structures.
Concepts of the Functional Matrix Hypothesis
-
Functional Matrices:
- The hypothesis posits that the growth of the craniofacial skeleton
is guided by the functional matrices surrounding it. These matrices
include:
- Muscles: The muscles of mastication, facial expression, and other soft tissues exert forces on the bones, influencing their growth and development.
- Soft Tissues: The presence and tension of soft tissues, such as the lips, cheeks, and tongue, can affect the position and growth of the underlying skeletal structures.
- Functional Activities: Activities such as chewing, swallowing, and speaking create functional demands that influence the growth patterns of the craniofacial complex.
- The hypothesis posits that the growth of the craniofacial skeleton
is guided by the functional matrices surrounding it. These matrices
include:
-
Growth and Development:
- According to the Functional Matrix Hypothesis, the growth of the craniofacial skeleton is not a direct result of genetic programming but is instead a response to the functional demands placed on it. This means that changes in function can lead to changes in growth patterns.
- For example, if a child has a habit of mouth breathing, the lack of proper nasal function can lead to altered growth of the maxilla and mandible, resulting in malocclusion or other dental issues.
-
Orthodontic Implications:
- The Functional Matrix Hypothesis has significant implications for
orthodontic treatment and craniofacial orthopedics. It suggests that:
- Functional Appliances: Orthodontic appliances that modify function (such as functional appliances) can be used to influence the growth of the jaws and improve occlusion.
- Early Intervention: Early orthodontic intervention may be beneficial in guiding the growth of the craniofacial complex, especially in children, to prevent or correct malocclusions.
- Holistic Approach: Treatment should consider not only the teeth and jaws but also the surrounding soft tissues and functional activities.
- The Functional Matrix Hypothesis has significant implications for
orthodontic treatment and craniofacial orthopedics. It suggests that:
-
Clinical Applications:
- The Functional Matrix Hypothesis encourages clinicians to assess the functional aspects of a patient's oral and facial structures when planning treatment. This includes evaluating muscle function, soft tissue relationships, and the impact of habits (such as thumb sucking or mouth breathing) on growth and development.
Factors to Consider in Designing a Spring for Orthodontic Appliances
In orthodontics, the design of springs is critical for achieving effective tooth movement while ensuring patient comfort. Several factors must be considered when designing a spring to optimize its performance and functionality. Below, we will discuss these factors in detail.
1. Diameter of Wire
- Flexibility: The diameter of the wire used in the spring significantly influences its flexibility. A thinner wire will yield a more flexible spring, allowing for greater movement and adaptability.
- Force Delivery: The relationship between wire diameter and force delivery is crucial. A thicker wire will produce a stiffer spring, which may be necessary for certain applications but can limit flexibility.
2. Force Delivered by the Spring
-
Formula: The force (F) delivered by a spring can be expressed by the formula: [ $$F \propto \frac{d^4}{l^3} $$] Where:
- ( F ) = force applied by the spring
- ( d ) = diameter of the wire
- ( l ) = length of the wire
-
Implications: This formula indicates that the force exerted by the spring is directly proportional to the fourth power of the diameter of the wire and inversely proportional to the cube of the length of the wire. Therefore, small changes in wire diameter can lead to significant changes in force delivery.
3. Length of Wire
- Flexibility and Force: Increasing the length of the wire decreases the force exerted by the spring. Longer springs are generally more flexible and can remain active for extended periods.
- Force Reduction: By doubling the length of the wire, the force can be reduced by a factor of eight. This principle is essential when designing springs for specific tooth movements that require gentler forces.
4. Patient Comfort
- Design Considerations: The design, shape, size, and force generation of the spring must prioritize patient comfort. A well-designed spring should not cause discomfort or irritation to the oral tissues.
- Customization: Springs may need to be customized to fit the individual patient's anatomy and treatment needs, ensuring that they are comfortable during use.
5. Direction of Tooth Movement
- Point of Contact: The direction of tooth movement is determined by the point of contact between the spring and the tooth. Proper placement of the spring is essential for achieving the desired movement.
- Placement Considerations:
- Palatally Placed Springs: These are used for labial (toward the lips) and mesio-distal (toward the midline) tooth movements.
- Buccally Placed Springs: These are employed when the tooth needs to be moved palatally and in a mesio-distal direction.
Headgear is an extraoral orthodontic appliance used to correct dental and skeletal discrepancies, particularly in growing patients. It is designed to apply forces to the teeth and jaws to achieve specific orthodontic goals, such as correcting overbites, underbites, and crossbites, as well as guiding the growth of the maxilla (upper jaw) and mandible (lower jaw). Below is an overview of headgear, its types, mechanisms of action, indications, advantages, and limitations.
Types of Headgear
-
Class II Headgear:
- Description: This type is used primarily to correct Class II malocclusions, where the upper teeth are positioned too far forward relative to the lower teeth.
- Mechanism: It typically consists of a facebow that attaches to the maxillary molars and is anchored to a neck strap or a forehead strap. The appliance applies a backward force to the maxilla, helping to reposition it and/or retract the upper incisors.
-
Class III Headgear:
- Description: Used to correct Class III malocclusions, where the lower teeth are positioned too far forward relative to the upper teeth.
- Mechanism: This type of headgear may use a reverse-pull face mask that applies forward and upward forces to the maxilla, encouraging its growth and improving the relationship between the upper and lower jaws.
-
Cervical Headgear:
- Description: This type is used to control the growth of the maxilla and is often used in conjunction with other orthodontic appliances.
- Mechanism: It consists of a neck strap that connects to a facebow, applying forces to the maxilla to restrict its forward growth while allowing the mandible to grow.
-
High-Pull Headgear:
- Description: This type is used to control the vertical growth of the maxilla and is often used in cases with deep overbites.
- Mechanism: It features a head strap that connects to the facebow and applies upward and backward forces to the maxilla.
Mechanism of Action
- Force Application: Headgear applies extraoral forces to
the teeth and jaws, influencing their position and growth. The forces can be
directed to:
- Restrict maxillary growth: In Class II cases, headgear can help prevent the maxilla from growing too far forward.
- Promote maxillary growth: In Class III cases, headgear can encourage forward growth of the maxilla.
- Reposition teeth: By applying forces to the molars, headgear can help align the dental arches and improve occlusion.
Indications for Use
- Class II Malocclusion: To correct overbites and improve the relationship between the upper and lower teeth.
- Class III Malocclusion: To promote the growth of the maxilla and improve the occlusal relationship.
- Crowding: To create space for teeth by retracting the upper incisors.
- Facial Aesthetics: To improve the overall facial profile and aesthetics by modifying jaw relationships.
Advantages of Headgear
- Non-Surgical Option: Provides a way to correct skeletal discrepancies without the need for surgical intervention.
- Effective for Growth Modification: Particularly useful in growing patients, as it can influence the growth of the jaws.
- Improves Aesthetics: Can enhance facial aesthetics by correcting jaw relationships and improving the smile.
Limitations of Headgear
- Patient Compliance: The effectiveness of headgear relies heavily on patient compliance. Patients must wear the appliance as prescribed (often 12-14 hours a day) for optimal results.
- Discomfort: Patients may experience discomfort or soreness when first using headgear, which can affect compliance.
- Adjustment Period: It may take time for patients to adjust to wearing headgear, and they may need guidance on how to use it properly.
- Limited Effectiveness in Adults: While headgear is effective in growing patients, its effectiveness may be limited in adults due to the maturity of the skeletal structures.
Myofunctional Appliances
- Myofunctional appliances are removable or fixed devices that aim to correct dental and skeletal discrepancies by promoting proper oral and facial muscle function. They are based on the principles of myofunctional therapy, which focuses on the relationship between muscle function and dental alignment.
-
Mechanism of Action:
- These appliances work by encouraging the correct positioning of the tongue, lips, and cheeks, which can help guide the growth of the jaws and the alignment of the teeth. They can also help in retraining oral muscle habits that may contribute to malocclusion, such as thumb sucking or mouth breathing.
Types of Myofunctional Appliances
-
Functional Appliances:
- Bionator: A removable appliance that encourages forward positioning of the mandible and helps in correcting Class II malocclusions.
- Frankel Appliance: A removable appliance that modifies the position of the dental arches and improves facial aesthetics by influencing muscle function.
- Activator: A functional appliance that promotes mandibular growth and corrects dental relationships by positioning the mandible forward.
-
Tongue Retainers:
- Devices designed to maintain the tongue in a specific position, often used to correct tongue thrusting habits that can lead to malocclusion.
-
Mouthguards:
- While primarily used for protection during sports, certain types of mouthguards can also be designed to promote proper tongue posture and prevent harmful oral habits.
-
Myobrace:
- A specific type of myofunctional appliance that is used to correct dental alignment and improve oral function by encouraging proper tongue posture and lip closure.
Indications for Use
- Malocclusions: Myofunctional appliances are often indicated for treating Class II and Class III malocclusions, as well as other dental alignment issues.
- Oral Habits: They can help in correcting harmful oral habits such as thumb sucking, tongue thrusting, and mouth breathing.
- Facial Growth Modification: These appliances can be used to influence the growth of the jaws in growing children, promoting a more favorable dental and facial relationship.
- Improving Oral Function: They can enhance functions such as chewing, swallowing, and speech by promoting proper muscle coordination.
Advantages of Myofunctional Appliances
- Non-Invasive: Myofunctional appliances are generally non-invasive and can be a more comfortable option for patients compared to fixed appliances.
- Promotes Natural Growth: They can guide the natural growth of the jaws and teeth, making them particularly effective in growing children.
- Improves Oral Function: By retraining oral muscle function, these appliances can enhance overall oral health and function.
- Aesthetic Appeal: Many myofunctional appliances are less noticeable than traditional braces, which can be more appealing to patients.
Limitations of Myofunctional Appliances
- Compliance Dependent: The effectiveness of myofunctional appliances relies heavily on patient compliance. Patients must wear the appliance as prescribed for optimal results.
- Limited Scope: While effective for certain types of malocclusions, myofunctional appliances may not be suitable for all cases, particularly those requiring significant tooth movement or surgical intervention.
- Adjustment Period: Patients may experience discomfort or difficulty adjusting to the appliance initially, which can affect compliance.
Twin Block appliance is a removable functional orthodontic device designed to correct malocclusion by positioning the lower jaw forward. It consists of two interlocking bite blocks, one for the upper jaw and one for the lower jaw, which work together to align the teeth and improve jaw relationships.
Features of the Twin Block Appliance
-
Design: The Twin Block consists of two separate components that fit over the upper and lower teeth, promoting forward movement of the lower jaw.
-
Functionality: It utilizes the natural bite forces to gradually shift the lower jaw into a more favorable position, addressing issues like overbites and jaw misalignments.
-
Material: Typically made from acrylic, the appliance is custom-fitted to ensure comfort and effectiveness during treatment.
Treatment Process
-
Initial Consultation:
- A comprehensive evaluation is conducted, including X-rays and impressions to assess the alignment of teeth and jaws.
-
Fitting the Appliance:
- Once ready, the Twin Block is fitted and adjusted to the patient's mouth. Initial discomfort may occur but usually subsides quickly.
-
Active Treatment Phase:
- Patients typically wear the appliance full-time for about 12 to 18 months, with regular check-ups for adjustments.
-
Retention Phase:
- After active treatment, a retainer may be required to maintain the new jaw position while the bone stabilizes.
Benefits of the Twin Block Appliance
-
Non-Surgical Solution: Offers a less invasive alternative to surgical options for correcting jaw misalignments.
-
Improved Functionality: Enhances chewing, speaking, and overall jaw function by aligning the upper and lower jaws.
-
Facial Aesthetics: Contributes to a more balanced facial profile, boosting self-esteem and confidence.
-
Faster Results: Compared to traditional braces, the Twin Block can provide quicker corrections, especially in growing patients.
Care and Maintenance
-
Oral Hygiene: Patients should maintain good oral hygiene by brushing and flossing regularly, especially around the appliance.
-
Food Restrictions: Avoid hard, sticky, or chewy foods that could damage the appliance.
-
Regular Check-Ups: Attend scheduled appointments to ensure the appliance is functioning correctly and to make necessary adjustments.
