NEET MDS Lessons
Orthodontics
Orthodontic Force Duration
-
Continuous Forces:
- Definition: Continuous forces are applied consistently over time without interruption.
- Application: Many extraoral appliances, such as headgear, are designed to provide continuous force to the teeth and jaws. This type of force is essential for effective tooth movement and skeletal changes.
- Example: A headgear may be worn for 12-14 hours a day to achieve the desired effects on the maxilla or mandible.
-
Intermittent Forces:
- Definition: Intermittent forces are applied in a pulsed or periodic manner, with breaks in between.
- Application: Some extraoral appliances may use intermittent forces, but this is less common. Intermittent forces can be effective in certain situations, but continuous forces are generally preferred for consistent tooth movement.
- Example: A patient may be instructed to wear an appliance for a few hours each day, but this is less typical for extraoral devices.
Force Levels
-
Light Forces:
- Definition: Light forces are typically in the range of 50-100 grams and are used to achieve gentle tooth movement.
- Application: Light forces are ideal for orthodontic treatment as they minimize discomfort and reduce the risk of damaging the periodontal tissues.
- Example: Some extraoral appliances may be designed to apply light forces to encourage gradual movement of the teeth or to modify jaw relationships.
-
Moderate Forces:
- Definition: Moderate forces range from 100-200 grams and can be used for more significant tooth movement or skeletal changes.
- Application: These forces can be effective in achieving desired movements but may require careful monitoring to avoid discomfort or adverse effects.
- Example: Headgear that applies moderate forces to the maxilla to correct Class II malocclusions.
-
Heavy Forces:
- Definition: Heavy forces exceed 200 grams and are typically used for rapid tooth movement or significant skeletal changes.
- Application: While heavy forces can lead to faster results, they also carry a higher risk of complications, such as root resorption or damage to the periodontal ligament.
- Example: Some extraoral appliances may apply heavy forces for short periods, but this is generally not recommended for prolonged use.
Orthopaedic appliances in dentistry are devices used to modify the growth of the jaws and align teeth by applying specific forces. These appliances utilize light orthodontic forces (50-100 grams) for tooth movement and orthopedic forces to induce skeletal changes, effectively guiding dental and facial development.
Orthopaedic appliances are designed to correct skeletal discrepancies and improve dental alignment by applying forces to the jaws and teeth. They are particularly useful in growing patients to influence jaw growth and positioning.
-
Types of Orthopaedic Appliances:
- Headgear: Used to correct overbites and underbites by applying force to the upper jaw.
- Protraction Face Mask: Applies anterior force to the maxilla to correct retrusion.
- Chin Cup: Restricts forward and downward growth of the mandible.
- Functional Appliances: Such as the Herbst appliance, which helps in correcting overbites by repositioning the jaw.
Mechanisms of Action
- Force Application: Orthopaedic appliances apply heavy forces (300-500 grams) to the skeletal structures, which can alter the magnitude and direction of bone growth.
- Anchorage: These appliances often use teeth as handles to transmit forces to the underlying skeletal structures, requiring adequate anchorage from extraoral sites like the skull or neck.
- Intermittent Forces: The use of intermittent heavy forces is crucial, as it allows for skeletal changes while minimizing dental movement.
Indications for Use
- Skeletal Malocclusions: Effective for treating Class II and Class III malocclusions.
- Growth Modification: Used to guide the growth of the maxilla and mandible in children and adolescents.
- Space Management: Helps in creating space for proper alignment of teeth and preventing crowding.
Advantages of Orthopaedic Appliances
- Non-Surgical Option: Provides a non-invasive alternative to surgical interventions for correcting skeletal discrepancies.
- Guides Growth: Can effectively guide the growth of the jaws, leading to improved facial aesthetics and function.
- Versatile Applications: Suitable for a variety of orthodontic issues, including overbites, underbites, and crossbites.
Limitations of Orthopaedic Appliances
- Patient Compliance: The success of treatment heavily relies on patient adherence to wearing the appliance as prescribed.
- Discomfort: Patients may experience discomfort or difficulty adjusting to the appliance initially.
- Limited Effectiveness: May not be suitable for all cases, particularly those requiring significant tooth movement or complex surgical corrections.
Headgear is an extraoral orthodontic appliance used to correct dental and skeletal discrepancies, particularly in growing patients. It is designed to apply forces to the teeth and jaws to achieve specific orthodontic goals, such as correcting overbites, underbites, and crossbites, as well as guiding the growth of the maxilla (upper jaw) and mandible (lower jaw). Below is an overview of headgear, its types, mechanisms of action, indications, advantages, and limitations.
Types of Headgear
-
Class II Headgear:
- Description: This type is used primarily to correct Class II malocclusions, where the upper teeth are positioned too far forward relative to the lower teeth.
- Mechanism: It typically consists of a facebow that attaches to the maxillary molars and is anchored to a neck strap or a forehead strap. The appliance applies a backward force to the maxilla, helping to reposition it and/or retract the upper incisors.
-
Class III Headgear:
- Description: Used to correct Class III malocclusions, where the lower teeth are positioned too far forward relative to the upper teeth.
- Mechanism: This type of headgear may use a reverse-pull face mask that applies forward and upward forces to the maxilla, encouraging its growth and improving the relationship between the upper and lower jaws.
-
Cervical Headgear:
- Description: This type is used to control the growth of the maxilla and is often used in conjunction with other orthodontic appliances.
- Mechanism: It consists of a neck strap that connects to a facebow, applying forces to the maxilla to restrict its forward growth while allowing the mandible to grow.
-
High-Pull Headgear:
- Description: This type is used to control the vertical growth of the maxilla and is often used in cases with deep overbites.
- Mechanism: It features a head strap that connects to the facebow and applies upward and backward forces to the maxilla.
Mechanism of Action
- Force Application: Headgear applies extraoral forces to
the teeth and jaws, influencing their position and growth. The forces can be
directed to:
- Restrict maxillary growth: In Class II cases, headgear can help prevent the maxilla from growing too far forward.
- Promote maxillary growth: In Class III cases, headgear can encourage forward growth of the maxilla.
- Reposition teeth: By applying forces to the molars, headgear can help align the dental arches and improve occlusion.
Indications for Use
- Class II Malocclusion: To correct overbites and improve the relationship between the upper and lower teeth.
- Class III Malocclusion: To promote the growth of the maxilla and improve the occlusal relationship.
- Crowding: To create space for teeth by retracting the upper incisors.
- Facial Aesthetics: To improve the overall facial profile and aesthetics by modifying jaw relationships.
Advantages of Headgear
- Non-Surgical Option: Provides a way to correct skeletal discrepancies without the need for surgical intervention.
- Effective for Growth Modification: Particularly useful in growing patients, as it can influence the growth of the jaws.
- Improves Aesthetics: Can enhance facial aesthetics by correcting jaw relationships and improving the smile.
Limitations of Headgear
- Patient Compliance: The effectiveness of headgear relies heavily on patient compliance. Patients must wear the appliance as prescribed (often 12-14 hours a day) for optimal results.
- Discomfort: Patients may experience discomfort or soreness when first using headgear, which can affect compliance.
- Adjustment Period: It may take time for patients to adjust to wearing headgear, and they may need guidance on how to use it properly.
- Limited Effectiveness in Adults: While headgear is effective in growing patients, its effectiveness may be limited in adults due to the maturity of the skeletal structures.
Transpalatal Arch (TPA) is an orthodontic appliance used primarily in the upper arch to provide stability, maintain space, and facilitate tooth movement. It is a fixed appliance that connects the maxillary molars across the palate, and it is commonly used in various orthodontic treatments, particularly in conjunction with other appliances.
Components of the Transpalatal Arch
-
Main Wire:
- The TPA consists of a curved wire that spans the palate, typically made of stainless steel or a similar material. The wire is shaped to fit the contour of the palate and is usually 0.036 inches in diameter.
-
Attachments:
- The ends of the wire are attached to the bands or brackets on the maxillary molars. These attachments can be soldered or welded to the bands, ensuring a secure connection.
-
Adjustment Mechanism:
- Some TPAs may include loops or bends that can be adjusted to apply specific forces to the teeth, allowing for controlled movement.
Functions of the Transpalatal Arch
-
Stabilization:
- The TPA provides anchorage and stability to the posterior teeth, preventing unwanted movement during orthodontic treatment. It helps maintain the position of the molars and can prevent them from drifting.
-
Space Maintenance:
- The TPA can be used to maintain space in the upper arch, especially after the premature loss of primary molars or in cases of crowding.
-
Tooth Movement:
- The appliance can facilitate the movement of teeth, particularly the molars, by applying gentle forces. It can be used to correct crossbites or to expand the arch.
-
Support for Other Appliances:
- The TPA can serve as a support structure for other orthodontic appliances, such as expanders or functional appliances, enhancing their effectiveness.
Indications for Use
- Space Maintenance: To hold space for permanent teeth when primary teeth are lost prematurely.
- Crossbite Correction: To help correct posterior crossbites by repositioning the molars.
- Arch Expansion: In conjunction with other appliances, the TPA can assist in expanding the dental arch.
- Stabilization During Treatment: To provide anchorage and prevent unwanted movement of the molars during orthodontic treatment.
Advantages of the Transpalatal Arch
- Fixed Appliance: Being a fixed appliance, the TPA does not require patient compliance, ensuring consistent force application.
- Versatility: The TPA can be used in various treatment scenarios, making it a versatile tool in orthodontics.
- Minimal Discomfort: Generally, the TPA is well-tolerated by patients and does not cause significant discomfort.
Limitations of the Transpalatal Arch
- Limited Movement: The TPA primarily affects the molars and may not be effective for moving anterior teeth.
- Adjustment Needs: While the TPA can be adjusted, it may require periodic visits to the orthodontist for modifications.
- Oral Hygiene: As with any fixed appliance, maintaining oral hygiene can be more challenging, and patients must be diligent in their oral care.
Frankel appliance is a functional orthodontic device designed to guide facial growth and correct malocclusions. There are four main types: Frankel I (for Class I and Class II Division 1 malocclusions), Frankel II (for Class II Division 2), Frankel III (for Class III malocclusions), and Frankel IV (for specific cases requiring unique adjustments). Each type addresses different dental and skeletal relationships.
The Frankel appliance is a removable orthodontic device that plays a crucial role in the treatment of various malocclusions. It is designed to influence the growth of the jaw and dental arches by modifying muscle function and promoting proper alignment of teeth.
Types of Frankel Appliances
-
Frankel I:
- Indications: Primarily used for Class I and Class II Division 1 malocclusions.
- Function: Helps in correcting overjet and improving dental alignment.
-
Frankel II:
- Indications: Specifically designed for Class II Division 2 malocclusions.
- Function: Aims to reposition the maxilla and improve the relationship between the upper and lower teeth.
-
Frankel III:
- Indications: Used for Class III malocclusions.
- Function: Encourages forward positioning of the maxilla and helps in correcting the skeletal relationship.
-
Frankel IV:
- Indications: Suitable for open bites and bimaxillary protrusions.
- Function: Focuses on creating space and improving the occlusion by addressing specific dental and skeletal issues.
Key Features of Frankel Appliances
-
Myofunctional Design: The appliance is designed to utilize the forces generated by muscle function to guide the growth of the dental arches.
-
Removable: Patients can take the appliance out for cleaning and during meals, which enhances comfort and hygiene.
-
Custom Fit: Each appliance is tailored to the individual patient's dental anatomy, ensuring effective treatment.
Treatment Goals
-
Facial Balance: The primary goal of using a Frankel appliance is to achieve facial harmony and balance by correcting malocclusions.
-
Functional Improvement: It promotes the establishment of normal muscle function, which is essential for long-term dental health.
-
Arch Development: The appliance aids in the development of the dental arches, providing adequate space for the eruption of permanent teeth.
Growth is the increase in size It may also be defined as the normal� change in the amount of living substance. eg. Growth is the quantitative aspect and measures in units of increase per unit of time.
Development
It is the progress towards maturity (Todd). Development may be defined as natural sequential series of events between fertilization of ovum and adult stage.
Maturation
It is a period of stabilization brought by growth and development.
CEPHALOCAUDAL GRADIENT OF GROWTH
This simply means that there is an axis of increased growth extending from the head towards feet. At about 3rd month of intrauterine life the head takes up about 50% of total body length. At this stage cranium is larger relative to face. In contrast the limbs are underdeveloped.�
By the time of birth limbs and trunk have grown faster than head and the entire proportion of the body to the head has increased. These processes of growth continue till adult.��
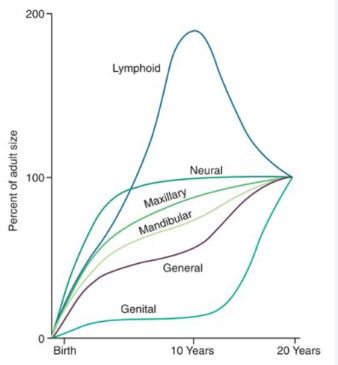
SCAMMON�S CURVE
In normal growth pattern all the tissue system of the body do not growth at the same rate. Scammon�s curve for growth shows 4 major tissue system of the body;
� Neural
� Lymphoid�
� General: Bone, viscera, muscle.
� Genital
The graph indicates the growth of the neural tissue is complete by 6-7 year of age. General body tissue show an �S� shaped curve with showing of rate during childhood and acceleration at puberty. Lymphoid tissues proliferate to its maximum in late childhood and undergo involution. At the same time growth of the genital tissue accelerate rapidly.�
�
Relapse
Definition: Relapse refers to the tendency of teeth to return to their original positions after orthodontic treatment. This can occur due to various factors, including the natural elasticity of the periodontal ligament, muscle forces, and the influence of oral habits.
Causes of Relapse
- Elasticity of the Periodontal Ligament: After orthodontic treatment, the periodontal ligament may still have a tendency to revert to its original state, leading to tooth movement.
- Muscle Forces: The forces exerted by the lips, cheeks, and tongue can influence tooth positions, especially if these forces are not balanced.
- Growth and Development: In growing patients, changes in jaw size and shape can lead to shifts in tooth positions.
- Non-Compliance with Retainers: Failure to wear retainers as prescribed can significantly increase the risk of relapse.
Prevention of Relapse
- Consistent Retainer Use: Adhering to the retainer regimen as prescribed by the orthodontist is crucial for maintaining tooth positions.
- Regular Follow-Up Visits: Periodic check-ups with the orthodontist can help monitor tooth positions and address any concerns early.
- Patient Education: Educating patients about the importance of retention and the potential for relapse can improve compliance with retainer wear.
