NEET MDS Lessons
Orthodontics
Anchorage in orthodontics refers to the resistance to unwanted tooth movement during orthodontic treatment. It is a critical concept that helps orthodontists achieve desired tooth movements while preventing adjacent teeth or the entire dental arch from shifting. Proper anchorage is essential for effective treatment planning and execution, especially in complex cases where multiple teeth need to be moved simultaneously.
Types of Anchorage
-
Absolute Anchorage:
- Definition: This type of anchorage prevents any movement of the anchorage unit (the teeth or structures providing support) during treatment.
- Application: Used when significant movement of other teeth is required, such as in cases of molar distalization or when correcting severe malocclusions.
- Methods:
- Temporary Anchorage Devices (TADs): Small screws or plates that are temporarily placed in the bone to provide stable anchorage.
- Extraoral Appliances: Devices like headgear that anchor to the skull or neck to prevent movement of certain teeth.
-
Relative Anchorage:
- Definition: This type allows for some movement of the anchorage unit while still providing enough resistance to achieve the desired tooth movement.
- Application: Commonly used in cases where some teeth need to be moved while others serve as anchors.
- Methods:
- Brackets and Bands: Teeth can be used as anchors, but they may move slightly during treatment.
- Class II or Class III Elastics: These can be used to create a force system that allows for some movement of the anchorage unit.
-
Functional Anchorage:
- Definition: This type utilizes the functional relationships between teeth and the surrounding structures to achieve desired movements.
- Application: Often used in conjunction with functional appliances that guide jaw growth and tooth positioning.
- Methods:
- Functional Appliances: Such as the Herbst or Bionator, which reposition the mandible and influence the growth of the maxilla.
Factors Influencing Anchorage
- Tooth Position: The position and root morphology of the anchorage teeth can affect their ability to resist movement.
- Bone Quality: The density and health of the surrounding bone can influence the effectiveness of anchorage.
- Force Magnitude and Direction: The amount and direction of forces applied during treatment can impact the stability of anchorage.
- Patient Compliance: Adherence to wearing appliances as prescribed is crucial for maintaining effective anchorage.
Clinical Considerations
- Treatment Planning: Proper assessment of anchorage needs is essential during the treatment planning phase. Orthodontists must determine the type of anchorage required based on the specific movements needed.
- Monitoring Progress: Throughout treatment, orthodontists should monitor the anchorage unit to ensure it remains stable and that desired tooth movements are occurring as planned.
- Adjustments: If unwanted movement of the anchorage unit occurs, adjustments may be necessary, such as changing the force system or utilizing additional anchorage methods.
Anterior Crossbite
Anterior crossbite is a dental condition where one or more of the upper front teeth (maxillary incisors) are positioned behind the lower front teeth (mandibular incisors) when the jaws are closed. This misalignment can lead to functional issues, aesthetic concerns, and potential wear on the teeth. Correcting anterior crossbite is essential for achieving proper occlusion and improving overall dental health.
Methods to Correct Anterior Crossbite
-
Acrylic Incline Plane:
- Description: An acrylic incline plane is a removable appliance that can be used to guide the movement of the teeth. It is designed to create a ramp-like surface that encourages the maxillary incisors to move forward.
- Mechanism: The incline plane helps to reposition the maxillary teeth by providing a surface that directs the teeth into a more favorable position during function.
-
Reverse Stainless Steel Crown:
- Description: A reverse stainless steel crown can be used in cases where the anterior teeth are significantly misaligned. This crown is designed to provide a stable and durable solution for correcting the crossbite.
- Mechanism: The crown can be adjusted to help reposition the maxillary teeth, allowing them to move into a more normal relationship with the mandibular teeth.
-
Hawley Retainer with Recurve Springs:
- Description: A Hawley retainer is a removable orthodontic appliance that can be modified with recurve springs to correct anterior crossbite.
- Mechanism: The recurve springs apply gentle pressure to the maxillary incisors, tipping them forward into a more favorable position relative to the mandibular teeth. This appliance is comfortable, easily retained, and predictable in its effects.
-
Fixed Labial-Lingual Appliance:
- Description: A fixed labial-lingual appliance is a type of orthodontic device that is bonded to the teeth and can be used to correct crossbites.
- Mechanism: This appliance works by applying continuous forces to the maxillary teeth, tipping them forward and correcting the crossbite. It may include a vertical removable arch for ease of adjustment and recurve springs to facilitate movement.
-
Vertical Removable Arch:
- Description: This appliance can be used in conjunction with other devices to provide additional support and adjustment capabilities.
- Mechanism: The vertical removable arch allows for easy modifications and adjustments, helping to jump the crossbite by repositioning the maxillary teeth.
Growth is the increase in size It may also be defined as the normal� change in the amount of living substance. eg. Growth is the quantitative aspect and measures in units of increase per unit of time.
Development
It is the progress towards maturity (Todd). Development may be defined as natural sequential series of events between fertilization of ovum and adult stage.
Maturation
It is a period of stabilization brought by growth and development.
CEPHALOCAUDAL GRADIENT OF GROWTH
This simply means that there is an axis of increased growth extending from the head towards feet. At about 3rd month of intrauterine life the head takes up about 50% of total body length. At this stage cranium is larger relative to face. In contrast the limbs are underdeveloped.�
By the time of birth limbs and trunk have grown faster than head and the entire proportion of the body to the head has increased. These processes of growth continue till adult.��
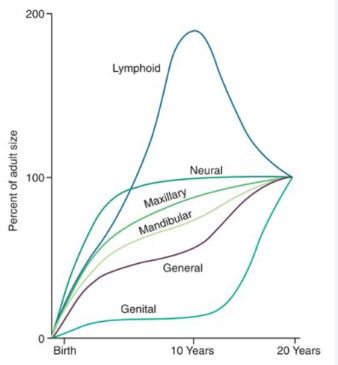
SCAMMON�S CURVE
In normal growth pattern all the tissue system of the body do not growth at the same rate. Scammon�s curve for growth shows 4 major tissue system of the body;
� Neural
� Lymphoid�
� General: Bone, viscera, muscle.
� Genital
The graph indicates the growth of the neural tissue is complete by 6-7 year of age. General body tissue show an �S� shaped curve with showing of rate during childhood and acceleration at puberty. Lymphoid tissues proliferate to its maximum in late childhood and undergo involution. At the same time growth of the genital tissue accelerate rapidly.�
�
Bruxism
Bruxism is the involuntary grinding or clenching of teeth, often occurring during sleep (nocturnal bruxism) or while awake (awake bruxism). It can lead to various dental and health issues, including tooth wear, jaw pain, and temporomandibular joint (TMJ) disorders.
Etiology
-
Central Nervous System (CNS):
- Bruxism has been observed in individuals with neurological conditions such as cerebral palsy and mental retardation, suggesting a CNS component to the phenomenon.
-
Psychological Factors:
- Emotional disturbances such as anxiety, stress, aggression, and feelings of hunger can contribute to the tendency to grind teeth. Psychological stressors are often linked to increased muscle tension and bruxism.
-
Occlusal Discrepancy:
- Improper interdigitation of teeth, such as malocclusion or misalignment, can lead to bruxism as the body attempts to find a comfortable bite.
-
Systemic Factors:
- Nutritional deficiencies, particularly magnesium (Mg�⁺) deficiency, have been associated with bruxism. Magnesium plays a role in muscle function and relaxation.
-
Genetic Factors:
- There may be a hereditary component to bruxism, with a family history of the condition increasing the likelihood of its occurrence.
-
Occupational Factors:
- High-stress occupations or activities, such as being an overenthusiastic student or participating in competitive sports, can lead to increased clenching and grinding of teeth.
Clinical Features
- Tooth Wear: Increased wear on the occlusal surfaces of teeth, leading to flattened or worn-down teeth.
- Jaw Pain: Discomfort or pain in the jaw muscles, particularly in the masseter and temporalis muscles.
- TMJ Disorders: Symptoms such as clicking, popping, or locking of the jaw, as well as pain in the TMJ area.
- Headaches: Tension-type headaches or migraines may occur due to muscle tension associated with bruxism.
- Facial Pain: Generalized facial pain or discomfort, particularly around the jaw and temples.
- Gum Recession: Increased risk of gum recession and periodontal issues due to excessive force on the teeth.
Management
-
Adjunctive Therapy:
- Psychotherapy: Aimed at reducing emotional disturbances and stress that may contribute to bruxism. Techniques may include cognitive-behavioral therapy (CBT) or relaxation techniques.
- Pain Management:
- Ethyl Chloride: A topical anesthetic that can be injected into the TMJ area to alleviate pain and discomfort.
-
Occlusal Therapy:
- Occlusal Adjustment: Adjusting the occlusion to improve the bite and reduce bruxism.
- Splints:
- Volcanite Splints: These are custom-made occlusal splints that cover the occlusal surfaces of all teeth. They help reduce muscle tone and protect the teeth from wear.
- Night Guards: Similar to splints, night guards are worn during sleep to prevent grinding and clenching.
- Restorative Treatment: Addressing any existing dental issues, such as cavities or misaligned teeth, to improve overall dental health.
-
Pharmacological Management:
- Vapo Coolant: Ethyl chloride can be used for pain relief in the TMJ area.
- Local Anesthesia: Direct injection of local anesthetics into the TMJ can provide temporary relief from pain.
- Muscle Relaxants: Medications such as muscle tranquilizers or sedatives may be prescribed to help reduce muscle tension and promote relaxation.
Catalan's Appliance
Catalan's appliance, also known as the Catalan appliance or lower inclined bite plane, is an orthodontic device primarily used to correct anterior crossbites and manage dental arch relationships. It is particularly effective in growing children and adolescents, as it helps to guide the development of the dental arches and improve occlusion.
Indications for Use
-
Anterior Crossbite:
- The primary indication for Catalan's appliance is to correct anterior crossbites, where the upper front teeth are positioned behind the lower front teeth when the jaws are closed.
-
Space Management:
- It can be used to create space in the dental arch, especially when there is crowding or insufficient space for the eruption of permanent teeth.
-
Guiding Eruption:
- The appliance helps guide the eruption of the permanent teeth into a more favorable position, promoting proper alignment.
-
Facilitating Growth:
- It can assist in the growth of the maxilla and mandible, helping to achieve a more balanced facial profile.
Design and Features
-
Components:
- The Catalan's appliance typically consists of:
- Acrylic Base: A custom-fitted acrylic base that covers the lower anterior teeth.
- Inclined Plane: An inclined plane is incorporated into the appliance, which helps to reposition the anterior teeth by providing a surface for the teeth to occlude against.
- Retention Mechanism: The appliance is retained in the mouth using clasps or other anchorage methods to ensure stability during treatment.
- The Catalan's appliance typically consists of:
-
Customization:
- The appliance is custom-made for each patient based on their specific dental anatomy and treatment needs. This ensures a proper fit and effective function.
Mechanism of Action
-
Correction of Crossbite:
- The inclined plane of the Catalan's appliance exerts forces on the anterior teeth, encouraging them to move into a more favorable position. This helps to correct the crossbite by allowing the maxillary incisors to move forward relative to the mandibular incisors.
-
Space Creation:
- By repositioning the anterior teeth, the appliance can create additional space in the dental arch, facilitating the eruption of permanent teeth and improving overall alignment.
-
Guiding Eruption:
- The appliance helps guide the eruption of the permanent teeth by maintaining proper arch form and preventing unwanted movements of the teeth.
Mesial Shift in Dental Development
Mesial shift refers to the movement of teeth in a mesial (toward the midline of the dental arch) direction. This phenomenon is particularly relevant in the context of mixed dentition, where both primary (deciduous) and permanent teeth are present. Mesial shifts can be categorized into two types: early mesial shift and late mesial shift. Understanding these shifts is important for orthodontic treatment planning and predicting changes in dental arch relationships.
Early Mesial Shift
- Timing: Occurs during the mixed dentition phase, typically around 6-7 years of age.
- Mechanism:
- The early mesial shift is primarily due to the closure of primate spaces. Primate spaces are natural gaps that exist between primary teeth, particularly between the maxillary lateral incisors and canines, and between the mandibular canines and first molars.
- As the permanent first molars erupt, they exert pressure on the primary teeth, leading to the closure of these spaces. This pressure causes the primary molars to drift mesially, resulting in a shift of the dental arch.
- Clinical Significance:
- The early mesial shift helps to maintain proper alignment and spacing for the eruption of permanent teeth. It is a natural part of dental development and can influence the overall occlusion.
Late Mesial Shift
- Timing: Occurs during the mixed dentition phase, typically around 10-11 years of age.
- Mechanism:
- The late mesial shift is associated with the closure of leeway spaces after the shedding of primary second molars. Leeway space refers to the difference in size between the primary molars and the permanent premolars that replace them.
- When the primary second molars are lost, the adjacent permanent molars (first molars) can drift mesially into the space left behind, resulting in a late mesial shift.
- Clinical Significance:
- The late mesial shift can help to align the dental arch and improve occlusion as the permanent teeth continue to erupt. However, if there is insufficient space or if the shift is excessive, it may lead to crowding or malocclusion.
Orthopaedic appliances in dentistry are devices used to modify the growth of the jaws and align teeth by applying specific forces. These appliances utilize light orthodontic forces (50-100 grams) for tooth movement and orthopedic forces to induce skeletal changes, effectively guiding dental and facial development.
Orthopaedic appliances are designed to correct skeletal discrepancies and improve dental alignment by applying forces to the jaws and teeth. They are particularly useful in growing patients to influence jaw growth and positioning.
-
Types of Orthopaedic Appliances:
- Headgear: Used to correct overbites and underbites by applying force to the upper jaw.
- Protraction Face Mask: Applies anterior force to the maxilla to correct retrusion.
- Chin Cup: Restricts forward and downward growth of the mandible.
- Functional Appliances: Such as the Herbst appliance, which helps in correcting overbites by repositioning the jaw.
Mechanisms of Action
- Force Application: Orthopaedic appliances apply heavy forces (300-500 grams) to the skeletal structures, which can alter the magnitude and direction of bone growth.
- Anchorage: These appliances often use teeth as handles to transmit forces to the underlying skeletal structures, requiring adequate anchorage from extraoral sites like the skull or neck.
- Intermittent Forces: The use of intermittent heavy forces is crucial, as it allows for skeletal changes while minimizing dental movement.
Indications for Use
- Skeletal Malocclusions: Effective for treating Class II and Class III malocclusions.
- Growth Modification: Used to guide the growth of the maxilla and mandible in children and adolescents.
- Space Management: Helps in creating space for proper alignment of teeth and preventing crowding.
Advantages of Orthopaedic Appliances
- Non-Surgical Option: Provides a non-invasive alternative to surgical interventions for correcting skeletal discrepancies.
- Guides Growth: Can effectively guide the growth of the jaws, leading to improved facial aesthetics and function.
- Versatile Applications: Suitable for a variety of orthodontic issues, including overbites, underbites, and crossbites.
Limitations of Orthopaedic Appliances
- Patient Compliance: The success of treatment heavily relies on patient adherence to wearing the appliance as prescribed.
- Discomfort: Patients may experience discomfort or difficulty adjusting to the appliance initially.
- Limited Effectiveness: May not be suitable for all cases, particularly those requiring significant tooth movement or complex surgical corrections.
